It’s hardly novel to point this out, but the coronavirus has left great swaths of Canada’s economy in disarray. Nearly every occupation and endeavour has been touched in some profoundly negative − if not crippling − way. Yet this devastation has not been complete; some jobs seem to be thriving rather than suffering. Among the beneficiaries: caution-tape manufacturers, plexiglass barrier installers, medical supply vendors and, perhaps most significantly, public health officials.

As the most visible element of governmental efforts to explain the dangers of Covid-19 and to plan, enforce and market various preventative measures, public health officials everywhere have found themselves thrust firmly into the spotlight since March. Many public health officers are now more visible and more widely admired than the politicians they serve. Headlining this group are Drs. Theresa Tam, Deena Hinshaw and Bonnie Henry, respectively the chief public health officers of Canada, Alberta and British Columbia. All three have been broadly acknowledged by the media to be “public health heroes.” Trust in them and their compatriots stands at an astounding 80 percent, according to opinion polls, levels most politicians can only dream about. A Facebook fan page for Alberta’s Hinshaw has over 11,000 followers. There’s even a line of t-shirts featuring the trio.
Given the sheer weight of responsibility placed on their shoulders over the past several months, and the consequences of decisions that might later prove mistaken or unfounded, no one should begrudge these hard-working civil servants their time in the sun. Quite often they have simply provided a sympathetic human face during a difficult time. “It may sound corny, but I do believe that kindness and support and working together is what will get us through this,” Henry said last month about the possibility of a second wave of the coronavirus. A global pandemic is the precise reason why we have public health officers. And by and large, they have risen to the challenge.

That said, however, we should be mindful that whatever accolades they deserve for their current performances are not turned into blank cheques for future innovations and interruptions of normal, daily life once the pandemic finally recedes. We should also remember Lord Acton’s wisdom that it is human nature for people who are given power over others to wield that power ever-more broadly and forcefully. Covid-19 represents the first global quarantine of healthy populations in human history, and it was imposed in dozens of democracies almost entirely by decree, without political debate or formal legislation.
In recent decades, in fact, public health practitioners have shown a decidedly imaginative interest in moving far beyond the activities that were once at the core of their historical missions, and that have won them so much praise in recent months. Rather than focusing on the narrowly-defined goals of identifying, tracking and mitigating the risks of communicable diseases – of which Covid-19 is a textbook example − public health officials in Canada and around the world have been eagerly inserting themselves into a seemingly endless array of topics from corporate food production to international trade to income inequality to whether even one glass of wine with dinner is a good idea. Everything, it seems, is open to being declared a “public health issue.”

And so, regardless of the superhero/celebrity status currently conferred on them, we must guard against public health officials’ inherent urge to wander far from their original mandate into areas where they have little expertise – and no reason or right to intrude. With a real risk that their current popularity will embolden an even greater sense of public health activism, we may soon wish to consider a “quarantine order” for public health officials themselves: Please remain inside your area of competency at all times.
So Who Needs a Drink?
Outside pandemics, one of the chief preoccupations of public health officials today is the degree to which adults should be allowed to make personal decisions that contradict medical advice. That urge is still going strong. In April, after scolding smokers about their continued reliance on the demon weed, Alberta’s Hinshaw also used her daily press briefing to tsk-tsk residents about drinking: “It is also important that we limit drinking alcohol during this time.” Then in June she claimed to have proof Albertans were drinking too much. Citing reports of “sharp increases in the sales of wine, beer and liquor as well as cannabis since our public health measures were put in place,” Hinshaw suggested big problems would soon reveal themselves once things opened back up again. She was later forced to recant on this, since she apparently had no evidence to prove her case beyond anecdotal observations that some stores seemed busier than usual.
Drinking among Canadians aged 15-24 is in long-term decline, age of first drinking is down and fatal drunk driving accidents are near all-time lows. You’d think all this progress would cheer public health officials. But it is never enough.
The scene was far more chaotic in Prince Edward Island, where the province gave just 24 hours notice that it was shutting down all government-owned liquor stores in mid-March when the lockdown began. The predictable mad scramble to stockpile supplies by residents earned them the wrath of the Island’s public health officer, Dr. Heather Morrison, who declared herself “disappointed in Islanders’ response in the last three hours,” as the line-ups grew to Soviet Union-era lengths. “We have talked about social distancing. We have talked about the importance of staying home unless it’s essential. That appears to have been ignored,” Morrison stewed. Thankfully for Islanders, a handful of privately-owned agency stores on the Island have remained open, and a few government stores have since reopened.

Some U.S. states also tried to shut down liquor stores based on public health advice, only to open them up again once they realized the disaster they had unleashed. And in Europe, the World Health Organization in mid-April declared “access [to alcohol sales] should be restricted during lockdown.” An abiding urge towards prohibition is a perennial fixation within the public health community, regardless of the circumstances.
In her 2018 annual report, Canada’s Chief Public Health Officer Tam grimly referred to alcohol as “a legal, socially acceptable, mind altering substance” without any reference to the fact many Canadians find moderate alcohol consumption a pleasurable activity, or that all the trend lines suggest the vast majority of them are already making wise choices when it comes to booze. Drinking among Canadians aged 15-24 is in long-term decline, age of first drinking is down and fatal drunk driving accidents are near all-time lows. You would think all this progress would cheer our public health officials. But it is never enough.
A recent modelling study using B.C. data appears to offer new motivation for this puritanical streak in public health. “Basically if you are drinking any amount of alcohol, you’re increasing your risk of cancer,” the paper’s lead author told the Globe and Mail in June. This led the Globe’s editorial board to conclude “the safest level of alcohol use is none.” It’s the sort of narrow-minded conclusion public health officials are often promoting. But it’s a message so distorted as to be effectively false.

Yes, there is a modest increase in certain medical risks associated with alcohol use. However, moderate drinking is also associated with greater sociability and stronger interpersonal relationships. And this sort of activity typically leads to better health and a longer life. There is, in other words, a trade-off at play with alcohol consumption that requires a nuanced approach.
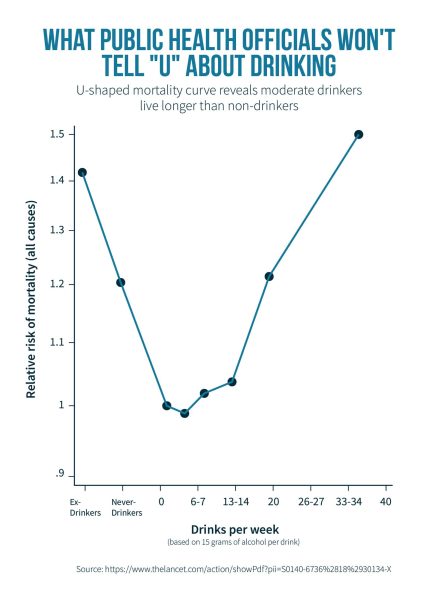
Consider a 2018 study in The Lancet, similar to the recent B.C. report, that also fixated on cancer rates and alcohol use, and that produced identical calls for total prohibition. Yet this report actually showed abstainers − both ex-drinkers and folks who have never touched a drop − have a higher relative mortality rate than moderate drinkers who get out and mingle more frequently. (See attached graph.) In fact, never-drinkers display an all-cause mortality rate equivalent to those who imbibe up to 24 drinks per week; the sweet spot for healthy living appears to be one or two drinks per day. Such a result ought to be considered information vital to the public’s health, but was instead hidden away in an appendix. No one in the public health field ever seems interested in discussing the health advantages of alcohol. Moderation, it seems, is never enough.
Will all these warnings about drinking during the lockdown (we called it “apocalypse sauce” in our house) translate into a renewed campaign of prohibition once the pandemic is over? That may depend on how much political capital public health officials have accumulated during their time in the spotlight. Consider it a trend to watch.
You Ain’t Going Nowhere
The impulse among public health officials to prefer overbroad rules rather than measured responses has been on full display throughout the pandemic. This was particularly evident in domestic travel restrictions that clearly violated Canadians’ mobility rights as enshrined in section 6 of the Canadian Charter of Rights and Freedoms.
In the milder cases, people weren’t actually legally confined and their rights technically weren’t violated. But the weight of the moral pressure was significant, and the frequent hectoring – typically amplified by panic-mongering news media – seemed to generate widespread confusion, with many people thinking that things had been prohibited when they were merely being discouraged. As recently as late June, Hinshaw was using her daily briefings to lecture Albertans on their travel plans, telling anyone with a cottage or camping spot in B.C. to stay put.
If the pandemic has proven anything, it’s that most public health officials subscribe to a rather narrow and tenuous definition of Canadians’ charter rights.
Elsewhere in the country, officials took it much farther. In some cases, municipal officials unilaterally discovered they possessed heretofore unknown dictatorial powers. In the southwestern Ontario municipality of Haldimand Norfolk, for example, the local medical officer of health instructed property owners that, “You are not permitted to occupy your secondary residence within the Health Unit, which includes a rented cottage, vacation home, beach house, chalet and/or condominium.” The fine for stepping foot onto your own property was set at $5,000. It was never made clear how municipalities, constitutionally creatures of the provinces with no actual law-making authority of their own, could freelance in this way.


Perhaps the most dramatic example came in Yukon, where the entire territory has been held in quarantine since March on the orders of the Chief Medical Officer of Health Dr. Brendan Hanley. Despite reporting no new cases since April, hundreds of travellers have been denied entry into the territory and those who have been allowed in must self-isolate for 14 days. Imposed by decree without formal debate or legislative approval, these restrictions (which will be lifted for visitors from B.C. Nunavut and the Northwest Territories on July 1) have devastated the local economy. The constitutionality of Hanley’s public health order has been rightly challenged by a group of Yukon businesses, as well as the Canadian Civil Liberties Association. If the pandemic has proven anything, it’s that most public health officials subscribe to a rather narrow and tenuous definition of Canadians’ constitutional rights.
Public Health the Way it Used to Be
Throughout Canada’s early history public health played a key role in creating a successful and stable country. Many of the most significant early improvements to the daily lives of Canadians can be ascribed to public health measures. For colonial-era governments, this was the creation of inspection and quarantine systems meant to protect existing populations from disease, such as cholera or smallpox, that could arrive via immigration. Later, medical breakthroughs allowed many of these diseases to be controlled or treated.
And as settlements grew to become towns and cities, public health boards were often the most important institutions offered by local government. Winnipeg’s first city hall meeting in 1874, for example, passed regulations against selling adulterated food and defiling water supplies. Plus every home was ordered to have a privy that was cleaned regularly, and animal carcasses had to be promptly removed from all city lots. These bylaws were backed by fines of up to $20, or 21 days in jail.


Clean water. Proper sewage treatment. Reliable food supplies. Control of communicable disease. These pedestrian-sounding efforts represent the foundation of modern society. And yet this traditional form of public health seems to have proven unsatisfying for its practitioners. It is now common practice to seek out policy areas far afield from these original, necessary pursuits. This may be due to institutional restlessness. Or perhaps it reflects the gradual infusion of progressive ideology into all academic topics. Regardless, since the mid-20th century, public health has moved on from its foundational concerns to tackle ever-grander and seemingly more politically-motivated goals.
Is Anything Not a Public Health Epidemic?
The fight against tobacco use has arguably been public health’s greatest modern achievement. Since then, all new campaigns have been measured against this standard of near-total compliance achieved through laws, taxes and public messaging. Aside from ongoing efforts to revive the prohibition of alcohol, obesity is another frequent fixation in this regard. Repeated calls for taxes on sodas, advertising bans, ingredient restrictions and a wide variety of other government interventions are meant to fundamentally alter the Canadian diet.

But while every puff of tobacco is a certifiable health hazard, food of all kind remains a necessity of life. Plus, the medical doctors making recommendations on fiscal measures to combat obesity have no understanding of the underlying economics at play. A vast preponderance of evidence reveals that taxes and other enforcement measures are incapable of producing the sort of wide-ranging dietary changes desired by their proponents. Perhaps the highest-profile expression of this controlling desire was New York City’s famous effort to get rid of large take-out soft drinks, the so-called Big Gulp Ban. This effort was properly quashed by the courts as being far beyond the remit of the city’s health department. It ought to be a cautionary tale. Unfortunately, it hasn’t worked out that way.
The sheer range of topics public health officials now claim to be within their purview is stunning in its breadth and boldness. In 2006 the public health department in Waterloo Region in southwestern Ontario, published a report bemoaning interregional trade in tomatoes. It declared the sale of any tomatoes sourced from outside the region to be an example of “redundant trade.”
It is also common for public health offices to assert the existence of “food swamps” – areas where convenience stores outnumber grocery stores − and to demand changes to local zoning laws to control the location of stores and fast food outlets. The promotion of local food and farmer’s markets is another popular public health crusade, as is vilification of corporate control of the food industry. And the Toronto Board of Health once had an opinion on the fact that Jenny McCarthy, a vocal opponent of vaccinations, had been named as a co-host of the American talk show The View. Even the programming decisions of daytime television now apparently fall within the scope of public health officials.
Such a sweeping mandate for public health is not a singular Canadian phenomenon. A 2015 ”Manifesto for the Public’s Health” published by the UK’s Faculty of Public Health declared nearly every possible issue of political significance – from obesity to traffic regulations to television content to alcohol use to child poverty to climate change − to be an issue requiring control by public health experts. “Introduce good laws to prevent bad health and save lives,” the manifesto declared.


If implemented, such a platform would entail near total control of nearly all personal life choices and economic levers by unelected public health officials who often seem to be indulging particularly strident ideological views. In 2012, a British Medical Journal article, Why Corporate Power is a Public Health Priority, appears to enlist the tobacco control trope in the service of Marxist aims. “Lethal though tobacco is, the harm being done to public health by our economic system is far greater,” the author intoned gravely.
Based on recent output of documents and declarations, the biggest prize of all for grasping public health officials is the debate over income inequality. It has become fashionable for public health officials to declare the gap between rich and poor to be their utmost concern. In 2013 the public health office in Waterloo Region released a study declaring the current concentration of wealth in Canada to be “socially corrosive” and requiring public health intervention. Similar reports have been issued by other cities, including Guelph, Toronto and Montreal, as well as by the Canadian Medical Association.
How many of us want to live in world where public health officials exert perpetual control over the economy, society and nearly all personal choices? In other words, who wants the Covid-19 clampdown to last forever?
A campaign by a public health organization Upstream astonishingly claims income inequality in Canada is responsible for “the premature deaths of 40,000 Canadians a year.” Although there is plenty of evidence that it is less healthy to be poor, the lack of any connection between the gap between rich and poor and health outcomes is easily demonstrated. Nonetheless, the notion remains surprisingly resilient, mainly because it opens up the possibility of public health oversight of almost all aspects of the economy.

The implications of modern public health’s grand economic designs was the subject of a highly contentious (within public health circles, at any rate) paper by University of Chicago law professor Richard Epstein in 2003 in the academic journal Perspectives in Biology and Medicine. Entitled Let the shoemaker stick to his last: A defense of the “old” public health”, Epstein detailed the great expansion of public health into the political realm during the late 20th century and the effect this has had on personal freedoms. “The designation of obesity as a public health epidemic is designed to signal that state coercion is appropriate,” he wrote of soda taxes, bans and the like. Of even greater concern, noted Epstein, is the incalculable and unmentioned cost associated with handing over control of the economy to a legion of activist-minded medical doctors untutored in the realm of fiscal policy or the nature of wealth creation:
“The modern public health makes every social change relevant to health issues. But once it opens up the field to examine…greater income equality, it must take into account the public health losses, now broadly defined, from the failure to create new wealth and maintain higher standards of living. At this point, the new public health is scarcely distinguishable from a general social welfarist position whose benefits it shares and whose fatal deficiencies it cannot escape.”
Epstein correctly challenges public health officials to take into account the full weight of consequences flowing from their efforts to exert control, including vast amounts of hidden economic damage as well as the erosion of social life, personal liberty and the bonds of inter-personal relations. All this has so far avoided proper attention. As for a requisite degree of humility in recognizing that there are limits to one’s genuine area of expertise – well, that seems to have simply never occurred to the entire field of public health.
But how many of us really want to live in world where public health officials can exert perpetual control over the economy, society, nearly all our personal choices and essentially every aspect of our lives? Who thinks, in other words, the Covid-19 clampdown should last forever?
When the Pandemic is Over
The past few months have been very good for the esteem of public health officials. When called upon, they largely delivered a competent and necessary service to the public. And for doing their duty, they deserve whatever applause is sent their way; all those t-shirts and Facebook fan pages can be considered reasonable compensation for services rendered. However, we must also be mindful that this adulation is in recognition of what Epstein calls “old public health” – the institution of public health that came into being in the 19th century because Canadians needed protection from communicable diseases. And as we have seen in 2020, that need has never gone away.
But we must also guard against any unnecessary or inappropriate expansion of those powers of persuasion and control into areas that lie far beyond the proper mandate of public health. We have already seen ample evidence of such inclinations, from over-broad restrictions on personal liberties to deliberately misleading narratives about alcohol use to claims about trade policy. There is clearly a great desire to expand the meaning of public health to cover an impossibly wide range of topics and areas far beyond the competency of the field.
For all these reasons, we should be prepared to lock down public health officials whenever they start acting in ways that threaten the economy, society or our freedoms as democratic citizens. After all, they didn’t hesitate to do the same thing to us.
Peter Shawn Taylor is senior features editor at C2C Journal. He lives in Waterloo, Ontario. This article was prepared with files from Anthony Furey.